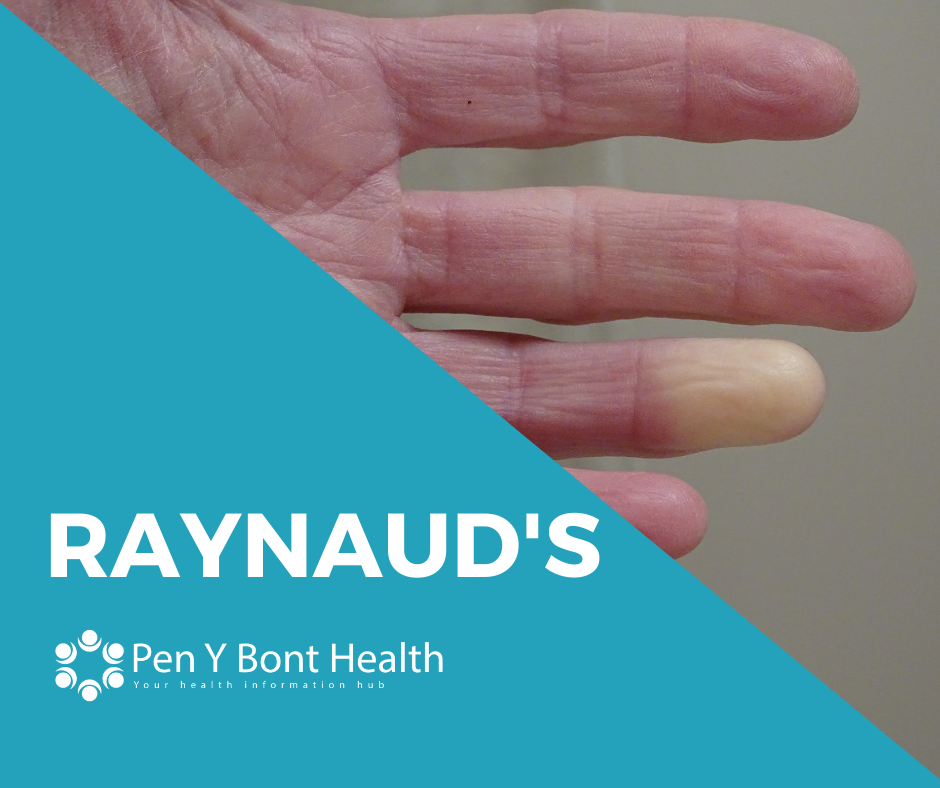
February is not only for Valentine’s Day, it is also the awareness month for Raynaud’s. Raynaud’s is an extremely common condition that is predicted to affect up to 10 million people in the UK.
What is Raynaud’s?
When someone has Raynaud’s, it means when their blood vessels narrow it is much more extreme than a normal response and results in the skin changing colour. When we are exposed to the cold a normal response of the body is for the blood vessels to become narrower – this is to minimise heat loss from the warm blood to preserve a standard core temperature. For those with Raynaud’s, their fingers and toes may change from white to blue and then to red. An attack of Raynaud’s can be very painful, especially as circulation begins to return to normal. It is common for Raynaud’s to affect the lips, nose, ears, and nipples in the same way.
What Causes Raynaud’s?
Raynaud’s occurs when blood vessels within the body’s extremities (furthest point away from the body’s core) such as fingers, toes and lips are over-sensitive. By having oversensitivity in these areas, a more extreme reaction is caused when exposed to certain triggers such as the cold weather. When this happens, it is known as a Raynaud’s attack.
Who is likely to develop Raynaud’s?
There is evidence to suggest that Raynaud’s can be inherited as it isn’t uncommon to see multiple cases within a family. Although we are unsure as to what exactly causes the condition, it is clear that it is not contagious and cannot be passed onto others. The condition is much more common in young women however it can still affect men, women, and children at any age.
Many people who have the condition do not see a doctor, however if you or someone you know suffers from regular cold hands and feet it is always worth talking it through with your GP. There are some autoimmune conditions such as scleroderma that increases your likelihood of developing Raynaud’s – this is because your immune system is overactive and attacks healthy tissue within your body.
Raynaud’s and Breastfeeding
Experiencing Raynaud’s when breastfeeding usually goes undiagnosed as it usually doesn’t last for long. However, this doesn’t mean it should go unspoken about as many new mothers can experience it. Raynaud’s can cause a deep pain in the breasts after feeding which many mothers automatically try to resolve by massaging them better or covering them up. Unfortunately, the symptoms are very similar to nipple thrush which causes misdiagnosis and the taking of thrush medication can make your Raynaud’s symptoms worse.
Most mothers who experience Raynaud’s have a history of having cold hands and feet or have a close relative who does. There are many treatments for Raynaud’s in breastfeeding mothers, so it is important to recognise your pain and talk to your midwife, health visitor or GP. It does not necessarily mean you should stop breastfeeding.
How to Treat Raynaud’s
There are multiple treatments available to help manage Raynaud’s. A few simple lifestyle changes can help lessen symptoms but if this doesn’t help then your GP will be able to recommend
treatments and medications. Avoiding repeated trauma to the fingertips through vibrating tools can massively help as well as limited your emotional stress.
Vitamin C and Vitamin E supplements are also recommended as their antioxidant can help protect the blood vessels from damage. Finally, there are options of prescribed medication you can take if the more natural remedies haven’t helped. These medications include Nifedipine, Diltiazem and Iloprost – your GP will be able to recommend the most suited option for you.
